


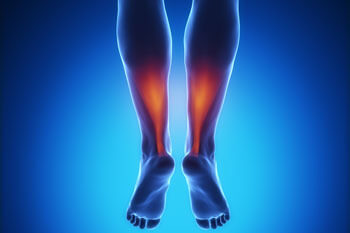
The Achilles tendon is the strongest tendon in the body and its function is to connect the calf muscles to the back of the heel. It is responsible for push-off in walking, running, and jumping. The calf muscles are made up of the deeper soleus and the more superficial gastrocnemius muscles, which conjoin distally to form the Achilles tendon.
The Achilles tendon has several areas where it may be injured. This may include the area where the calf muscle becomes the tendon called the musculotendinous junction. Blood supply comes from the soleus muscle and this injury heals fairly quickly. Another, area of frequent injury is the insertion of the Achilles tendon at the back of the heel. The blood supply at this area comes from the back of the heel bone. Also susceptible to injury is the thin “cord like” tendinous portion of the Achilles. This area has a poor blood supply and when injured, takes an extended time to heal.
The most common type of Achilles tendon problems occur insidiously in athletic people and include small tears within this tendon. A thickened area of the Achilles tendon, which sometimes feel like a nodule develops as the Achilles tries to heal and remodel itself. Without complete immobilization, this scarification continues causing more thickening.
Many patients present complaining of a painful bump at the back of the heel. X-rays in our office are taken, which usually reveals a calcium deposit or posterior heel spur. This prominent or bony overgrowth of bone can rub against the Achilles tendon at its insertion leading to inflammation or small tears.
Once a proper diagnosis is made by clinical examination and with assistance of diagnostic ultrasound or x-rays taken in our office, appropriate treatment can begin. Sometimes, an MRI is ordered to determine the extent of injury.
We often fit and dispense custom orthotics with deep heel cups to reduce the excessive teeter-totter and rocking of the heel bone, which reduces irritation of the Achilles tendon insertion at the back of the heel. Heel lifts may be used to reduce strain. We also utilize compression braces to help reduce swelling. When necessary, we perform homeopathic injections to the Achilles tendon to reduce inflammation. Cortisone injections are to be avoided. Enzyme injections maybe administered to help reduce nodules and scar tissue of the Achilles tendon. EPAT acoustic shockwave treatments are performed in our office to stimulate healing. This is used along with treatment by a physical therapist.
Unfortunately, in the middle aged and older population, the Achilles tendon may rupture causing significant pain and inability to walk. Patients have related to us that someone kicked them in the back of the leg but no one was present. Others felt a pop when they were playing sports. Sedentary patients may be treated with cast immobilization. However, our patient population is composed of extremely active individuals and for them Achilles ruptures usually necessitate immediate surgery.
Surgical intervention for acute ruptures includes end-to-end repair, but we typically reinforce the Achilles tendon with an allograft to ensure an extremely strong repair. This enhances our active patients return to full activity.
Please call our emergency number if you feel you have an acute rupture of the Achilles tendon.
To help prevent Achilles problems, it is important to stretch or massage the calf muscles to keep them flexible. Calf raises, leg presses, running, and jumping activities when properly performed are all exercises which can strengthen the Achilles tendon.
Should you have any pains to your Achilles or calf please schedule an appointment for a detailed examination and professional care.
Written by Richard T. Braver, DPM, FACFAS
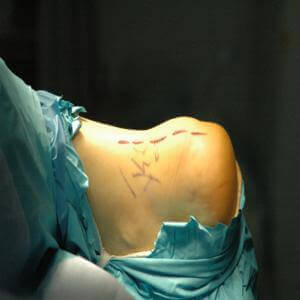
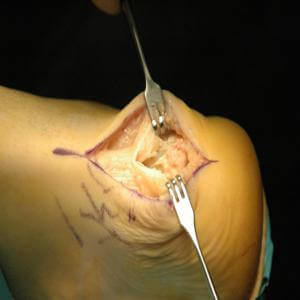
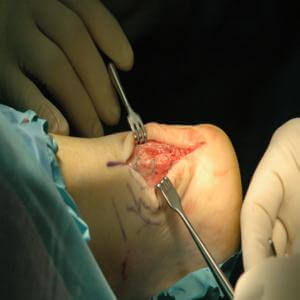
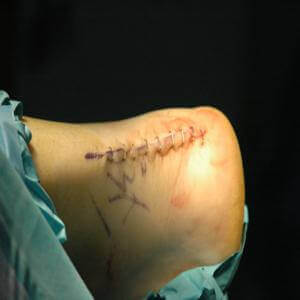
Photos courtesy of Richard T. Braver, DPM